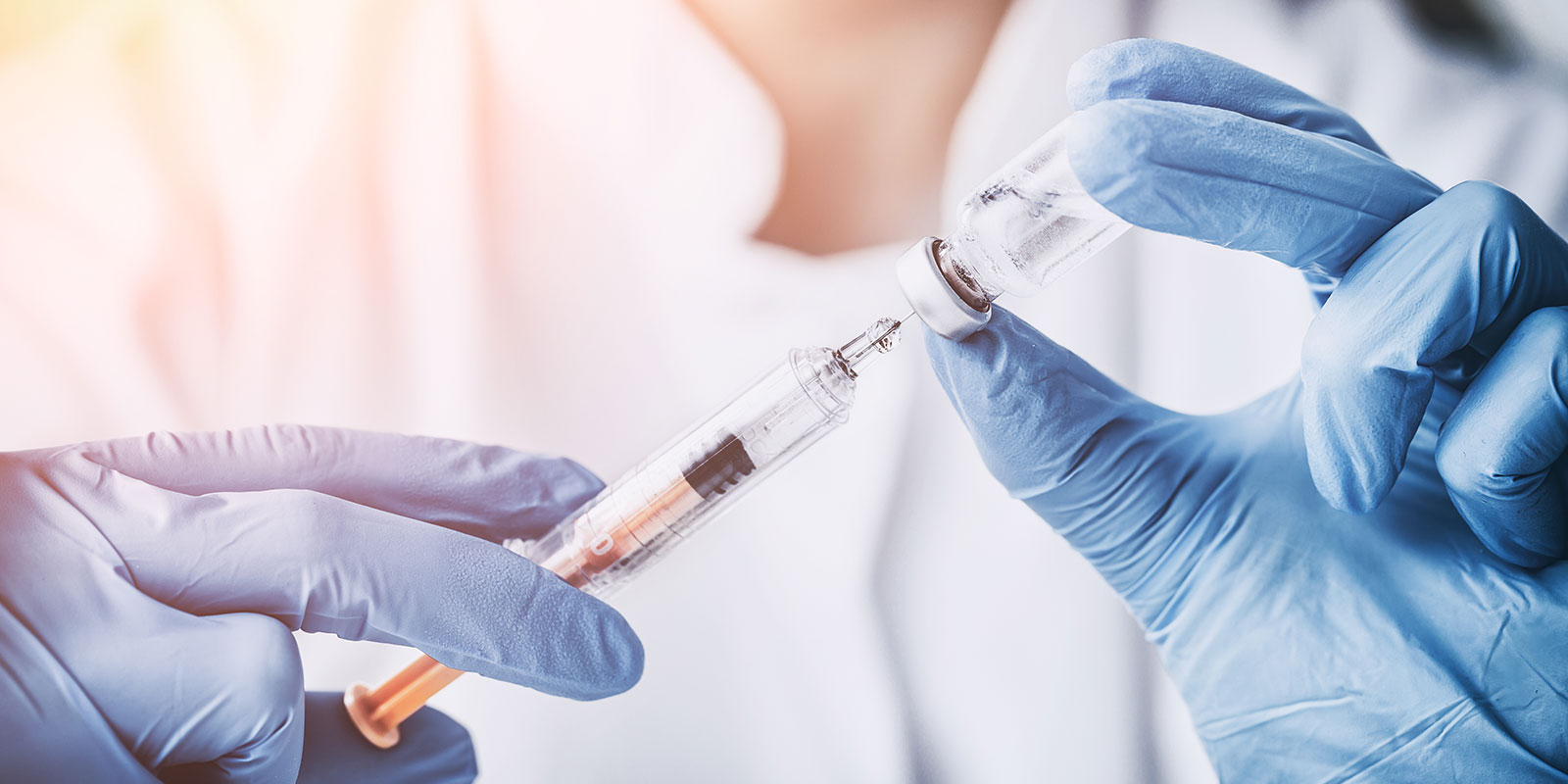
Back in 2002, in the midst of the SARS (Severe acute respiratory syndrome) outbreak, B.C. researchers like Brett Finlay were among the first to sequence the SARS genome and develop containment strategies.
Finlay, a professor in the faculty of medicine’s departments of biochemistry and molecular biology and microbiology and immunology, the Michael Smith Laboratories and a Peter Wall Distinguished Professor at UBC, is now part of a committee to advise the province on COVID-19 research priorities. This committee, coordinated by the Michael Smith Foundation for Health Research, will help answer questions like: What does the science tell us about how to ease restrictions? What can we learn from the way other countries have responded?
Finlay discusses his involvement in the development of three potential SARS vaccines, and how that experience can help inform our response to COVID-19.
Q: Why does it usually take so long to develop a vaccine?
A: First of all, you’ve got to be able to sequence and grow the virus, and that’s not always immediate. And then you have to wait to see an immune response, which takes usually at least a month. After this, you have to work your way up through different animal models, and then you’ve got to do human trials to make sure it’s safe to use in people.
What was tricky with SARS was you had to then use the vaccine in an area where the disease is endemic, in order to prove it actually works. That was hard in SARS because we didn’t know where it was going to flare up. And then you’ve got to do all the safety requirements associated with it.
The bottom line is if you put the pedal to the metal, you could probably get something to market within a year – this is about as fast as you can do it.

Brett Finlay
Q: What was the response during SARS to develop a vaccine?
A: SARS is a type of coronavirus like COVID-19. When SARS hit, no one knew anything about coronaviruses. But then, as you can imagine, just like COVID-19 now, everyone in the world was all over it. However, when SARS did not come back, the next year enthusiasm went out the window and rightly so — people moved on to other things.
Now, with COVID-19, my guess is it’s probably going to be here for the long term, and so I think there’s a significant market in terms of a vaccine. But let’s pretend you made a wonderful SARS vaccine the first year we had it, and then it never came back. Making vaccines is a $200 million to billion-dollar investment to get it out to the public.
Q: What are the components of a faster response learned during or since SARS?
A: In science, normally, you take it one step at a time. With SARS, what we learned is you should do things in parallel. You have already started to figure out where you’re going to do the field testing sites and what the animal models were, while you’re still just trying to grow the virus. So working in parallel can really streamline your timeline. Instead of having to wait for one thing to do, you assume you’re going to get to the next step, and then start down that line.
There were major hurdles too. First of all, our system is not built for rapid vaccine development; it usually takes 10 to 15 years to get a vaccine approved. So you are fighting the standard regulations — which are there for safety — but they’re very difficult. One thing that you can do is go straight into human trials if you can prove it works in two relevant animal models if the circumstance is really dire.
Q: Are there other lessons that can be taken from that development process and applied to COVID-19?
A: Technology has changed since we worked on SARS – you can work a lot quicker with RNA and DNA. But the same issues still apply. The other thing is you’re dealing with the immune system and we cannot predict what is going to make a good vaccine. It’s really a lot of trial and error. You think, we have MERS [Middle East Respiratory Syndrome] we have SARS and COVID-19, we’ve got all these respiratory coronaviruses, we’ve got animal vaccines for coronaviruses. Why can’t we just have a generic coronavirus vaccine and whatever comes along we just use the vaccine for the current virus? Unfortunately, the immune system doesn’t work like that.
You have to look at all the steps: where can they be sped up? Can we be proactive and have processes in place, like a clinical trial centre ready to go when the vaccine comes online? Who’s going to produce this? How do you scale up to vaccinate the entire world, pretty much overnight? These are the kind of issues you have to deal with.
Q: Do you have a gut feeling as to what our best shot will be, in terms of techniques or approaches to developing a coronavirus vaccine?
A: What we did with SARS, which no one else I know of in the world did, is we didn’t pick any one particular approach and put all our money in it. Instead we tried three parallel strategies to see which one would get us there. We were able to compare those three strategies head to head, so we had a much better idea at the end of six months about which technologies were going to work better.
So who knows? They’re trying RNA vaccines now – there’s no approved RNA vaccine out there but they’re trying that strategy. Unfortunately you just can’t pick a winner in terms of gut feelings. The best thing is, you try them all in parallel, you compare and contrast, and pick the best one.
A version of this story originally appeared on the Peter Wall Institute for Advanced Studies website.