The number of programs and prescribers offering safer supply to reduce risk of overdose increased dramatically in the early days of the COVID-19 pandemic, according to a new study looking at services across Canada.
The findings, published this month in the International Journal of Drug Policy, suggest capacity for further rapid scale-up of flexible safer supply prescribing to address the increasing toxic drug supply.

Dr. Stephanie Glegg
“Many public health experts anticipated that the early response to COVID-19 in March 2020 could lead to an increase in overdose and substance use-related harms,” says the study’s lead author Dr. Stephanie Glegg, a postdoctoral fellow at UBC’s department of medicine and the BC Centre on Substance Use (BCCSU). “Safer supply was identified as an option to reduce those risks and with new clinical guidance and policy changes introduced to support prescribing we witnessed a dramatic increase in both access and availability.”
As part of a national environmental scan, the researchers documented that 60 new sites were prescribing safer supply in May 2020, a 285-per-cent increase from the 21 sites available just two months earlier in March 2020. Through interviews with healthcare providers, the study authors found that the COVID-19 pandemic was a driving force behind this rapid scale-up in prescribing services.
Measures to limit COVID-19 spread have been cited as contributing to an increase in fatal drug poisonings and substance use related hospitalizations in regions across Canada, which led to disruptions to the global illicit drug supply chain, a reduction in the availability of harm reduction services, and more isolation to reduce risk of infection.
More access to safer supply but barriers still exist
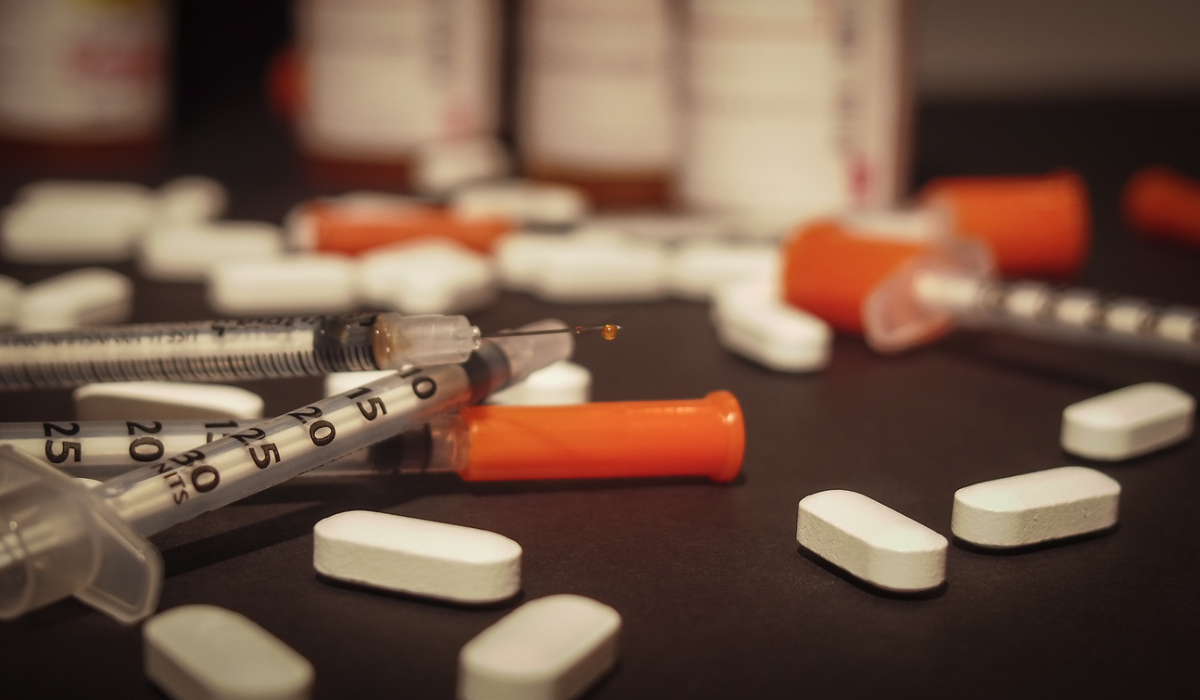
Safer supply refers to providing prescribed medications as an alternative to the toxic illegal drug supply to people who are at high risk of overdose. During COVID-19 the illicit drug supply has become increasingly toxic as fentanyl concentrations increase, and unpredictable with the emergence of contaminants such as benzodiazepines.
British Columbia saw the most dramatic expansion of sites and prescribers offering safer supply, with the number rising from two in March 2020 to 56 in May 2022.
“This expansion in B.C. was partially driven by interim provincial risk mitigation guidance published by the BCCSU,” said Dr. Glegg.
“With new clinical guidance and policy changes introduced to support prescribing we witnessed a dramatic increase in both access and availability.”
Dr. Stephanie Glegg
Provincial and regional bodies in Ontario and Québec also updated guidance for safer supply and COVID-19 risk mitigation prescribing in the months immediately following the declaration of the COVID-19 pandemic.
The researchers documented that the most common substances prescribed were opioids, made available mostly through addiction treatment programs, community health centres and primary care clinics, outreach and home delivery services, and onsite pharmacies models – relatively flexible program settings able to quickly adapt practices based on community need.
Despite the rapid increase in services, access is still limited and barriers to scaling up prescribed safer supply persist. Access in rural and remote settings remains mostly non-existent and 79 per cent of safer supply services were unfunded.
Fears of diversion remain a barrier to prescribing
Concerns related to the risk of diversion have also been cited as barrier to a broader scaling up of safer supply prescribing. Drug diversion is when prescription medications are distributed illicitly for purposes not intended by the prescriber.

Dr. Nadia Fairbairn
A perceived over-prescribing of pharmaceutical opioids in the early 2000s is often cited as a factor in the increase of opioid-related overdoses. However, data from various provincial coroners services indicates that prescription opioids have not been a key contributor to fatal overdose. Additionally, recent research has found that diverted prescription opioids can have a protective effect on community, as people become less reliant on the toxic illicit drug supply.
“As clinicians, we have a duty and an obligation to keep people safe even if it’s not within a treatment framework,” says the study’s senior author Dr. Nadia Fairbairn, an addiction medicine clinician and the Philip Owen Professor in Addiction Medicine at UBC. “It can be complex and challenging, to balance that obligation with the potential for opioid-naïve people to access diverted prescription opioids. The reluctance that many clinicians have about prescribing safer supply speaks to the need for other models of delivery.”
Other approaches to safer supply include public health prescribing models and community-led non-prescriber based models.
A summary of key findings from the study is available on the BCCSU website.