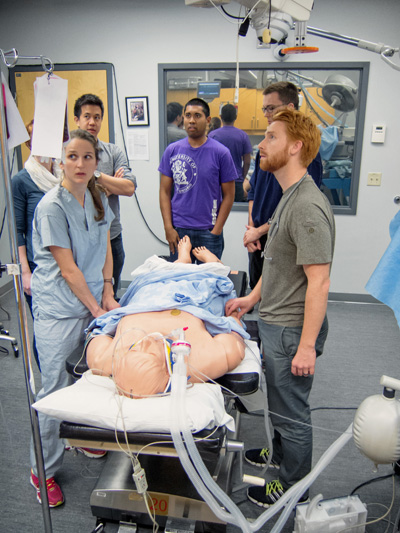
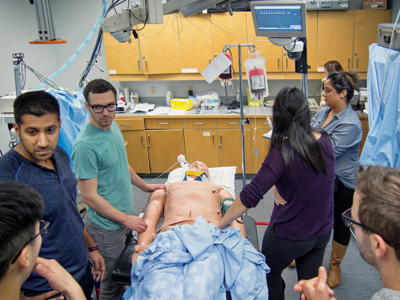
Kate Smith, an obstetrics-gynaecology resident, has noticed that the temperature of the critically injured trauma patient laid out on the table before her has fallen to a worrying 34 degrees. She calls out that information to the five or so other residents working alongside her, from other specialties – surgery, emergency medicine, anesthesiology. But none of them takes heed.
A few minutes later, Dr. Smith points it out again, suggesting they look at the patient’s temperature. Still no reaction. So, a few minutes after that, she suggests they apply a forced-air warming blanket. No one, including the team leader, follows her advice.
Into this seemingly disconcerting situation walks a senior resident, not to rescue the patient from hypothermia, but to hand out self-evaluation forms to the residents and usher them out of the room.
And the patient? Not to worry – it’s a simulation mannequin. No harm done.
During the subsequent debriefing session, faculty members and senior residents who observed the action behind a one-way mirror bring up Dr. Smith’s futile efforts to warm the patient. Rather than criticize the group, they praise Dr. Smith for trying, ever so diplomatically, to assert herself in a tense, somewhat chaotic environment.
“You have to find the appropriate point to tell the team leader, and you have to make sure you get your point across about how important it is,” says Naisan Garraway, a Clinical Assistant Professor of Surgery. “It’s good to address people by their names, and to say, ‘Here’s why I’m worried.’ You don’t want to be too confrontational, but you do want to take it up a level.”
This kind of feedback about team dynamics dominates the debriefings of this simulation course for residents, called Perioperative Emergency Management, or POEM. Although ample attention is paid to specific technical skills and knowledge – which lab tests should be ordered, which drugs should be given or avoided, whether a patient should be intubated – there is as much if not more discussion of crisis resource management, or CRM.
Breaking down silos
Developed by the aviation industry after its realization that most crashes were due to teamwork failure leading to human error, CRM emphasizes such principles as “flattening the hierarchy,” “closed-loop communication,” and “situational awareness” — issues and skills usually absent from the textbooks.

Related story: Practice until perfect
How an expanded, resident-led simulation program at BC Children’s Hospital is boosting trainee performance
These skills are particularly relevant when health professionals with different areas of expertise — not just physicians, but nurses and respiratory therapists — are called upon to deal with the frequent emergencies that arise. Yet residents do most of their simulation training in silos defined by the medical profession’s specialties.
“Surgeons train with surgeons, anesthesiologists train with anesthesiologists,” says Clinical Assistant Professor Laine Bosma, the Director of the Anesthesia Simulation Program and the Faculty of Medicine’s co-lead on simulation for residents. “We generally don’t train them in a way that reflects the true reality of modern, team-based acute care.”
POEM was created to address that disconnect. Now in its fifth year, POEM’s innovative mixing of specialties in trauma simulation has attracted the attention of other medical schools. One of those observing the group this day was Douglas Smink, an Associate Professor of Surgery at Harvard Medical School.
He and his colleagues at Brigham and Women’s Hospital also have discovered the value of team simulation. But it mostly involves putting experienced faculty through their paces, because the hospital’s malpractice insurer, which is picking up the tab, feels that’s a better investment.
“We’re trying to figure out a way to do something like this with our residents,” says Dr. Smink, Associate Medical Director of the hospital’s simulation centre and director of its general surgery residency program. “It’s a really impressive program, and the fact that they got all these people here is fantastic. In an academic medical centre, to get all those groups in the same room at the same time is a real challenge.”
It wasn’t easy at UBC, either. It took a junior anesthesiology resident, Siu-Kae Yeong, to jump-start the project.
Dr. Yeong, when confronted by real emergencies early in her training, realized she wasn’t prepared for the challenges of working alongside residents in other fields, under high-stakes, high-pressure conditions.
“Each team player may have different ideas about the diagnosis or the management needed, and we may be wrong or we may be right,” she says. “How do we make appropriate clinical decisions and manage crises effectively to provide the best care for the patient?”
Fortunately, the table was already being set for a solution.
Back to the classroom
Morad Hameed, the then-director of UBC’s general surgery residency program, had launched a new course in 2010 – Surgical Competencies in Resuscitation and Stabilization for Hospital Patients, or CRASH. All general surgery, orthopaedics and urology residents were pulled from their rotations after just three months of training to spend an entire month in classrooms and simulation rooms, to front-load essential knowledge, foster teamwork, introudce junior residents to senior residents, and raise morale.
“First-year residents are among the earliest responders to crises in the hospital, and they face tremendous pressure and stress,” says Dr. Hameed, an Associate Professor of Surgery, and Head of the Section on Trauma and Acute Care Surgery. “The rationale for the CRASH course was to give them early mastery and confidence in their knowledge, their technical skills and their ability to follow and lead teams in complex, multidisciplinary health care environments. There are CRASH courses in surgical training programs all over North America, but no one was doing it for a month, and as comprehensively as we are.”
Within a few years of its debut, CRASH has been embraced by all surgical training programs at UBC, including neurosurgery, cardiac surgery, vascular surgery, plastic surgery, ear, nose and throat surgery, anesthesiology, emergency medicine and obstetrics and gynaecology.
But residents from the various specialties originally weren’t doing simulation training alongside each other, until Dr. Yeong began pushing for Anesthesiology and Emergency Medicine to join.
“I was very enthusiastic about simulating, but I never thought of simulation across disciplines, until Siu-Kae brought it to my attention,” Dr. Hameed says. “That’s when we started to notice the team dynamics. Even first-year residents were stuck in their own silos, and the teams didn’t have combined situational awareness.”
So Dr. Hameed and Dr. Yeong, along with various colleagues, including Ravi Sidhu, the Assistant Dean of Postgraduate Medical Education, and Sandra Jarvis-Selinger, the then-Assistant Dean of Curriculum, carved POEM out of CRASH. Dr. Bosma came along in 2012 with his expertise in simulation, and is now co-leading POEM with Sonia Butterworth, a Clinical Associate Professor in the Department of Surgery and the co-lead for residency simulation programs.
High-stakes skills, high-pressure communication
POEM brings together residents from those departments and a few others, sorts them into mixed groups of about six, and runs them through two, day-long sessions; one day revolves around a single patient going through five different stations, while the other involves five different patients. During each segment, an experienced nurse plays the role, not surprisingly, of an experienced nurse, feeding them simulated background on the patient, sometimes introducing a curve ball or two, sometimes pointing out something that cries out for their attention. After each station, they discuss with instructors and senior residents what they did right, what they did wrong, and what could have been done – or said – better.
Following the patient throughout the day allows the group to cover all of the specialties of the participating residents, from the ER to the imaging suite to the OR to the ICU. Residents take turns as the team leader.
On this particular day, the scenario begins with a 33-year-old man – played by the mannequin at VGH’s Centre of Excellence for Simulation Education and Innovation – brought to the hospital from a high-speed motor vehicle accident (MVA). He has a liver smash, lacerations to his bowel and a pelvic fracture – though the residents don’t know that at first.
“To summarize, we have a 33-year-old male who was in an MVA,” says Adrienne McKercher, a first-year obstetrics and gynaecology resident. “He came in responsive, but now he is non-responsive. We’re currently intubating. We have put in a chest tube on his right side, and he has equal air bilaterally. We’re going to intubate and continue from there.”
After ordering chest and pelvic X-rays, an ultrasound, and a CT scan (the latter suggested by the experienced nurse), giving him blood, and calling for a consult from orthopaedics as well as a forced-air warming blanket, they “log roll” the patient onto his side to examine his back side.
The observers were impressed with Dr. McKercher’s leadership – her frequent summarizing of the situation, her consistent use of first names, her diligence in “closing the loop” on exchanges, and her refraining from “task-overloading” any single person.
Lalitha Rupesinghe, a Clinical Associate Professor in Anesthesiology, Pharmacology and Therapeutics, also praised Dr. McKercher’s willingness to take suggestions that she hadn’t thought of, including ordering a nasogastric tube and a catheter.
“It’s great that you were open to it,” Dr. Rupesnighe says. “You’ll find in some codes you go to, the leader isn’t always receptive to having feedback. It’s really important that the people in the team feel comfortable coming to you and saying, ‘Have you thought of this?’ But you still have to be able to make up your own mind about the appropriate route to go. Think about how you respond to stressful situations. The more you become aware of how you respond, the more you will be able to temper that response.”